PROMAC Team Looking Forward To Reduction In Maternal And Neonatal Mortality
By: , June 22, 2020The Full Story
Project Coordinator of the Programme for the Reduction of Maternal and Child Mortality (PROMAC), Dr. Simone Spence, says the team is looking forward to seeing reductions in maternal and neonatal mortality and morbidity, based on all that the project has been able to achieve in trying to improve maternal outcomes in Jamaica.
According to Dr. Spence, the programme, which has been strengthening the overall public health system, seeks to assist Jamaica in attaining Millennium Development Goals Four and Five, now Sustainable Development Goal Three, and has been active since early 2014 following the signing of the financing agreement in November 2013.
She tells JIS News that the journey has been long and fulfilling and that the tangible outcomes have been many; however, the most important outcomes will be the overall reductions in maternal and child mortality and these will come with time.
“We are finally at that point where we have actually seen a number of milestones and achievements out of this project, which was funded by the EU to the tune of 22 million Euros (€22M), in partnership with the Government of Jamaica,” she says, adding that the programme is being managed by the Ministry of Health and Wellness, with the contracting authority being the Planning Institute of Jamaica (PIOJ).
Dr. Spence, who is also the Director of Health Promotion and Protection at the Ministry, outlines some of the achievements to date.
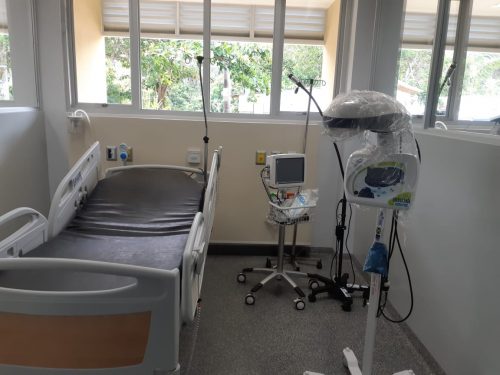
“Under Component One, which sought to address newborn and emergency obstetric care, we have developed 48 high-dependency spaces in maternal and neonatal High Dependency Units (HDUs) in four facilities across the country, namely St. Ann’s Bay Regional Hospital, Victoria Jubilee Hospital, Spanish Town Hospital and Bustamante Hospital for Children,” she notes.
She adds that equipment was procured for the HDUs at a cost of €3.6 million, while the amount expended on the construction of the HDUs was €9.6 million.
“Under Component Two, which looked at improving the quality of primary healthcare (health centres) and referral systems there, we would have procured six ambulances over the period as well as radiographic and ultrasound equipment, in order to strengthen diagnostic services,” Dr. Spence explains.
These, she says, were supplied along with fully equipped midwife bags to support the primary healthcare team, and this was done at a cost of €1.2 million.
Component Three, she adds, sought to look at clinical knowledge and augmenting the skills of healthcare workers.
“We would have trained over 230 doctors and nurses in specialised programmes at the University of the West Indies (UWI), as well as at the University of Technology (UTech), in areas such as the Doctor of Medicine (DM) programme, paediatrics, obstetrics and gynaecology, anaesthesia and intensive care,” she informs.
There have also been Fellowships, such as the Neonatalogy, Maternal and Foetal Medicine and Critical Care. Nurses were also trained in the Master of Science for Nursing Education programme, as well as in Fundamentals of Neonatal Ventilation, in order to support in-service training.
Dr. Spence points out that there was also training in nutrition, neonatal nursing and nutrition, critical care nursing and post basic midwifery.
“We have also trained over 1,000 primary healthcare workers in different areas in order to improve the quality of management of the high-risk pregnancies at both the primary and secondary care levels, and that was to the tune of €2 million,” she informs.
“Under Component Four, which looked at health-seeking behaviour of the targeted population and improving the role and effectiveness of civil society, we would have had partnerships with Rise Life Management and the National Family Planning Board (NFPB). These partnerships would have resulted in national campaigns used to raise awareness among the reproductive population,” Dr. Spence says.
She points out that Rise Life Management has executed the Healthy Baby, Healthy You campaign, which created awareness around nutrition, chronic illnesses and the importance of visiting the clinic, especially during the antenatal and postnatal periods.
Dr. Spence informs that the NFPB is about to launch two campaigns, titled ‘Clinic is a Must’ and ‘Healthy Body is a Must’, the latter aimed at encouraging women in the reproductive age group to be healthy in order to be pregnant. This, she says, is also intended to improve maternal and neonatal outcomes.
The Department of Community Health and Psychiatry at UWI, in partnership with the Women’s Resource Outreach Centre (WROC), has been charged with focusing on the rights of the mother and child, “so their main activities look at citizen mobilisation, organising civil society groups and looking at policies to support the rights of the mothers and their children, [and] so they had launched a media campaign with the slogan Know Your Health Rights,” she says, adding that the interventions will cost €1.3 million.
The institutional strengthening and capacity building of the Ministry of Health and Wellness has been done, both at the national and regional levels.
More than 100 staff members have been trained in project management, inventory management, financial and contractual procedures as well as strategic planning processes.
“So, over the life of this project we have done a lot. The project concludes November of this year and we’re just looking forward to actually seeing the results for our country. With the help of the EU, we put our money where our mouth is, put the MDGs and SDGs into action and moved to strengthen the public health system overall in order to provide quality care to this particular group of persons,” Dr. Spence says.
Meanwhile, Minister of Health and Wellness, Dr. the Hon. Christopher Tufton, in highlighting the merits of the programme, says PROMAC represents good news for high-risk pregnant women and premature babies in Jamaica based on PROMAC’s strategic objectives being built around attaining the United Nation MDGs, now SDGs, which focus on reducing maternal and child mortality ratios.
The Minister, who recently opened the St. Ann’s Bay Hospital HDU, points out that although the facility is the only one that has been officially opened, to date, construction of the HDUs at Victoria Jubilee Hospital, Bustamante Hospital for Children and Spanish Town Hospital have all been completed.

The St. Ann’s Bay Hospital facility includes a neonatal HDU with eight beds, two neonatal isolation suites and maternal HDU with five beds, including a maternal isolation suite.
All facilities will be equipped with highly specialised radiographic technology, digital computerised radiographic imaging systems, critical care ventilators and special patient-monitoring equipment.
EU Delegation Head, Ambassador Malgorzata Wasilewska, says that PROMAC is the first major EU-funded project in Jamaica that focuses on the health sector and specifically on maternal health.

She says that pregnancy and childbirth are essential to the existence of humanity and it is incumbent on governments and societies to ensure that every woman has a fair chance to have a healthy pregnancy and a safe delivery, no matter where in the world they live or their social background.
She commends the Ministry of Health and Wellness for its vision and the implementation and management of PROMAC.
“The outcomes of this huge effort are already visible but will be much higher once all the newly built and equipped high-dependency units start to operate and when there is a drastic reduction of the maternal and child mortality ratios,” she says.





